Strategic Revenue DesignsIdentify, Prevent, and Recapture Revenue Loss
Our clients agree that double-digit revenue losses are both recoverable and preventable.
Strategic Revenue Designs (SRD) identifies and recovers systemic revenue losses driven by payer reimbursement avoidance tactics and system-level misalignment between payer rules, billing logic, and contractual payment frameworks—often persisting beyond the capabilities of standard billing processes.
SRD bridges the gap between submitted claims, payer behavior, and actual reimbursement using a proprietary, AI-guided, expert-verified system that models contracts, analyzes claims at scale, and supports resolution with certified revenue cycle professionals. The result is measurable recovery of revenue that was earned but never captured.
What Makes SRD Different
Recovery beyond denials
SRD analyzes paid and closed claims, identifying underpayments hidden in contract variance, zero-pay claims, and payer behavior patterns that traditional billing operations overlook.
No workflow disruption
We operate alongside internal or third-party billing teams. No system replacement. No interruption to daily operations.
Root-cause intelligence
Our analysis exposes payer-specific issues, recurring human error, and contract ambiguity to reduce future revenue leakage.
Performance-aligned
SRD is paid based on recovered revenue. Our success is directly tied to yours.
AI-guided, Expert-verified
Our proprietary system uses AI to model complex reimbursement contracts and analyze claims at scale, while certified revenue cycle and coding experts oversee validation, escalation, and final resolution to ensure clinical, contractual, and financial accuracy.
The Underpayment Problem
7-10+% Revenue Leakage
The average provider loses roughly one-tenth of net patient revenue to systemic underpayment embedded in payer behavior, contract ambiguity, and claim adjudication.
Underpayments persist because:
• Payer tactics and billing rules continue to evolve
• Internal prevention at scale is virtually impossible
• Traditional vendors ignore zero-pay claims, sub-threshold variances, and long-cycle reviews
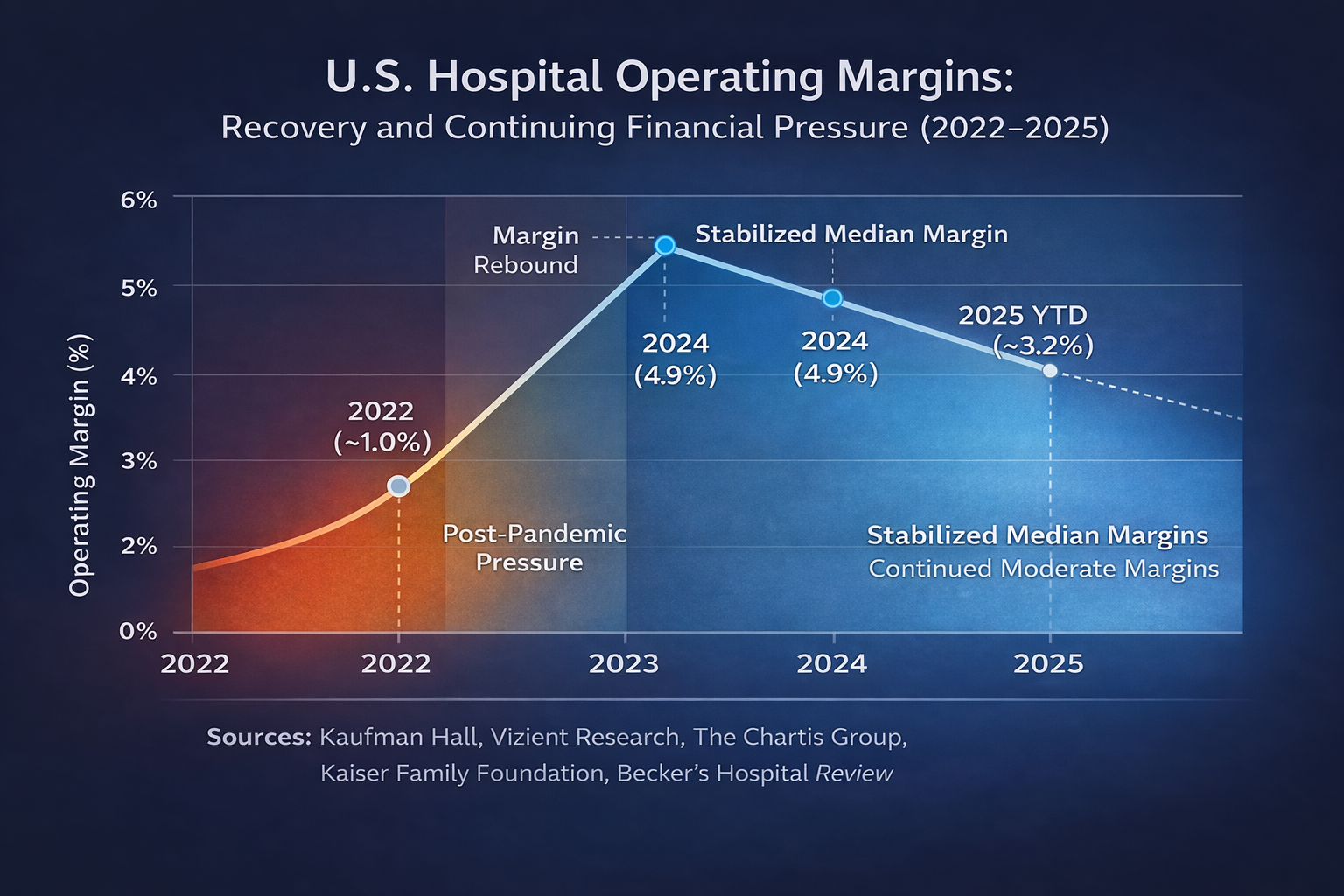
The result is chronic margin pressure—despite operational improvements elsewhere.
Where Revenue Is Lost
Revenue erosion compounds quietly across the reimbursement lifecycle.
Small variances at each step accumulate into material loss before revenue ever reaches the balance sheet.
Payer Coverage
SRD’s platform includes every major medical provider payer-specific module, covering:
Medicare
Medicare Advantage
Medicaid and Managed Medicaid
All major commercial payers
Each module incorporates payer-specific contracts, billing rules, and reimbursement logic, and is continuously updated to reflect evolving payer behavior.
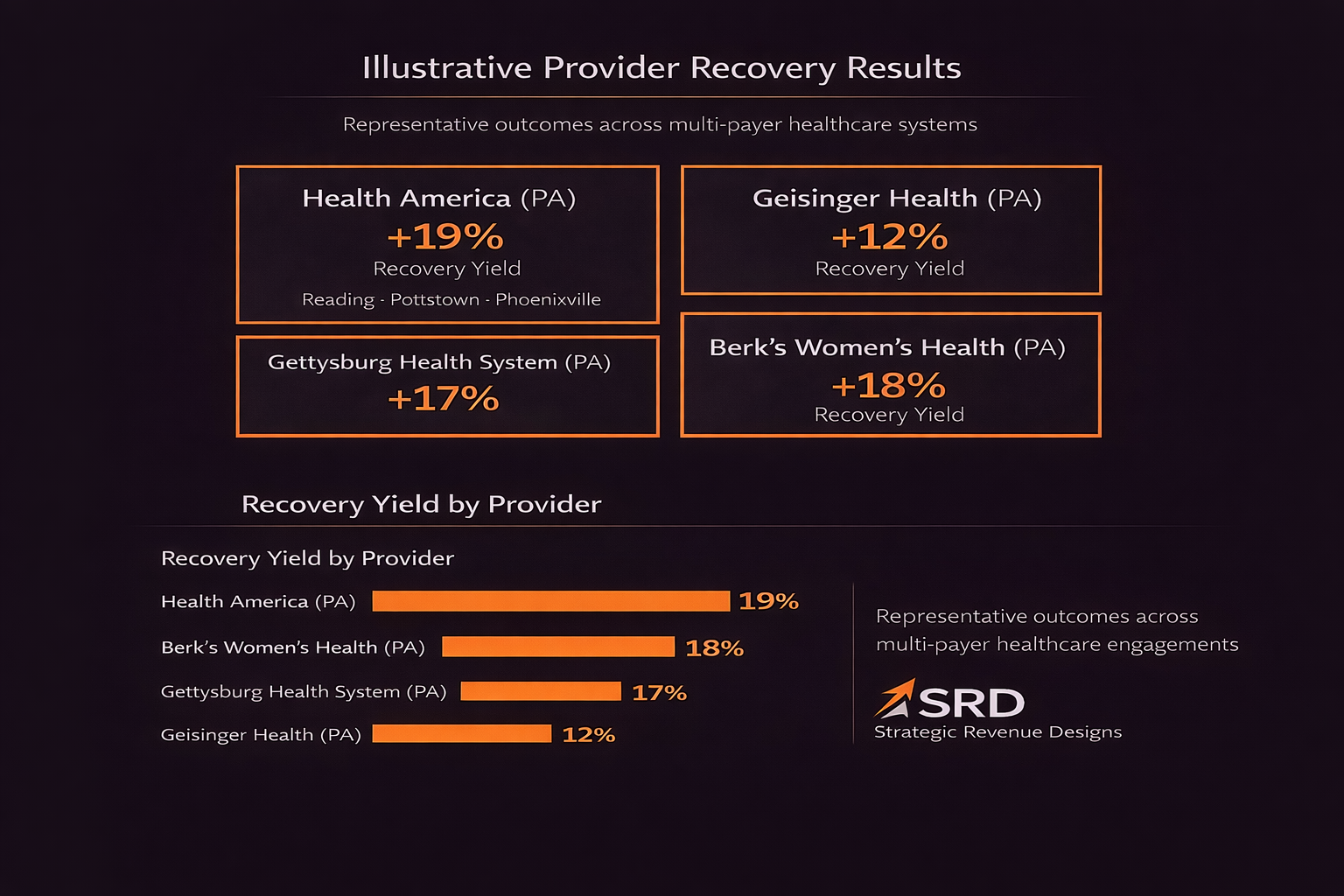
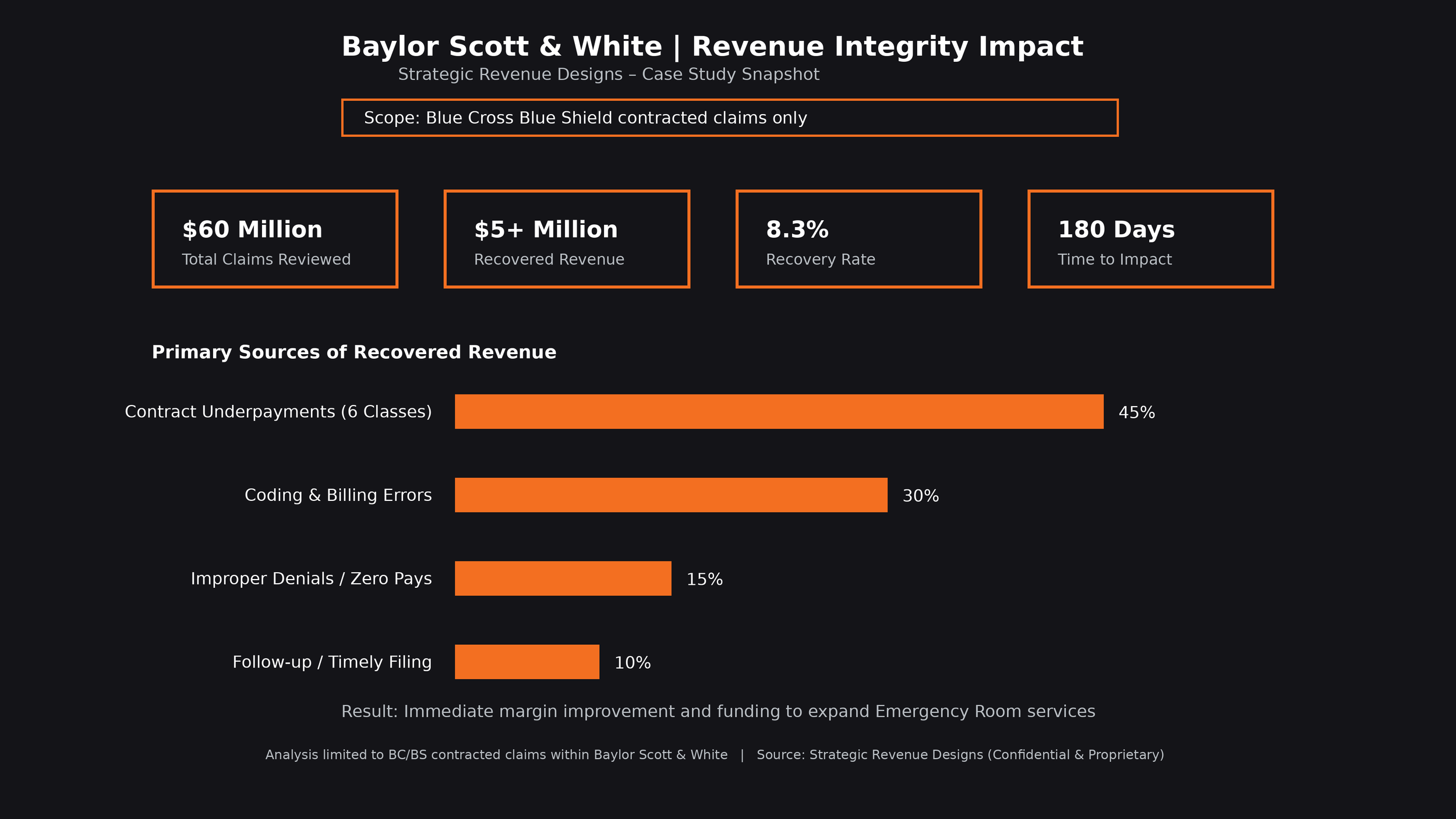
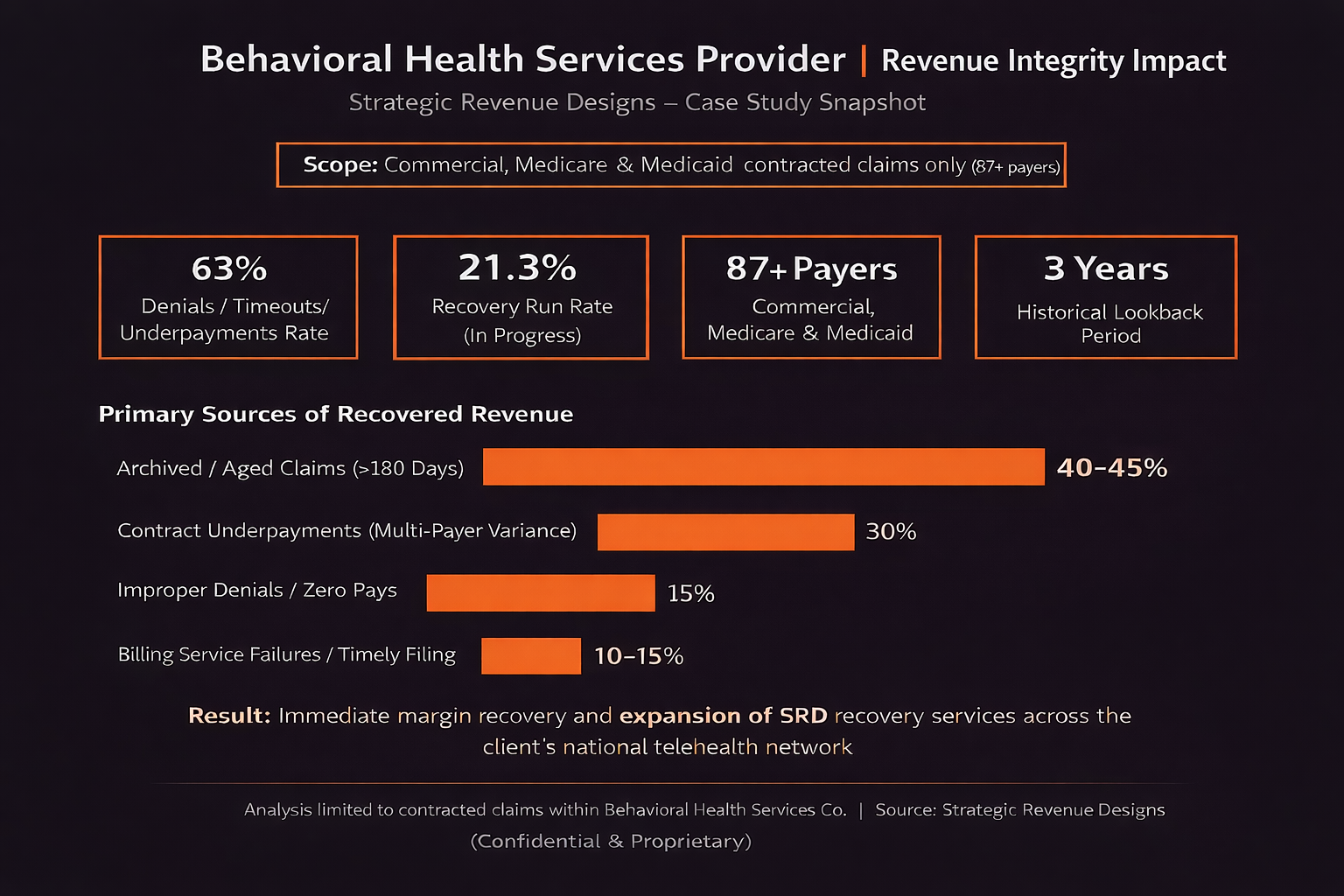
Representative Case Studies
SRD delivers measurable, verified recovery across diverse provider environments.
Compliance & Security
Fully HIPAA and PHI compliant
Secure, cloud-based infrastructure
Controlled access and encrypted data handling
Designed for enterprise healthcare environments
Data privacy and regulatory compliance are foundational to every SRD engagement.
The SRD Team
Scott Schickler
Founder & Chief Executive Officer
Scott Schickler brings more than 30 years of leadership across insurance, employee benefits, healthcare contracting, and federal health policy. A pioneer in pre-tax benefits and self-funded program design, and a former advisor during the Affordable Care Act era, Scott founded Strategic Revenue Designs to address healthcare’s most persistent challenge: payment integrity.
Contact Us
If recovering 7%–10+% of earned revenue is worth a conversation, we welcome the discussion.
Strategic Revenue Designs
4906 Penn Ave, Suite 201
South Heidelberg Township, PA 19608
Scott Kurtz
Executive Director
📧 scott.kurtz@strategicrevenuedesigns.com
📞 (858) 353-3437
Request a Preliminary Revenue Analysis
A high-level review designed to identify potential underpayment exposure and recovery opportunity.